 |
Home |
Fact Sheet on Secondhand Smoke |
| James. Repace, MSc., Physicist Repace Associates, Inc., Secondhand Smoke Consultants Bowie, Maryland 20720, U.S.A. Ichiro Kawachi, PhD, Associate Professor Stanton Glantz, PhD., Professor 9/1/99 |
 |
Home |
Fact Sheet on Secondhand Smoke |
| James. Repace, MSc., Physicist Repace Associates, Inc., Secondhand Smoke Consultants Bowie, Maryland 20720, U.S.A. Ichiro Kawachi, PhD, Associate Professor Stanton Glantz, PhD., Professor 9/1/99 |
Throughout the developed world, nations engage in the practice of pollution control with the intention of protecting human health against the effects of harmful chemical contaminants in food, water, and air. Accordingly, recognized standards of acceptability for harmful contaminants in food, beverages, drinking water, outdoor air, and indoor air in industrial workplaces has taken hold, and control measures appropriate for these different environments have evolved. However, in many workplaces, including offices, restaurants, and bars, SHS causes exposure to toxic chemicals not permitted in other environments.
This Fact Sheet explores SHS issues in the following areas: hazard, exposure, dose, dose-response, risk, and control.
Hazard: Epidemiological studies around the world have investigated whether passive smoking causes elevations in lung cancer, heart disease, and other diseases. These secondhand smoke epidemiological studies generally assess exposure using surrogate exposure variables such as spousal smoking. They also often suffer from the lack of a truly unexposed control group. These problems tend to obscure risks. Nevertheless, the epidemiological studies of passive smoking provide convincing evidence of the detection of an effect at environmental levels of exposure. The most powerful evidence of effect is the existence of dose-response relationships: of the 30 world studies of passive smoking & lung cancer extant in 1992, 14 reported a test for exposure-response, and 10 were statistically significant at the 95% confidence level (p<0.05) [U.S.EPA, 1992]. The probability of ten or more studies reaching this level by chance alone is less than 1 in ten billion. This evidence was sufficient for the U.S. Environmental Protection Agency to conclude that SHS was a "known human carcinogen." By 1997, the numbr of published epidemiological studies of lung cancer and passive smoking had increased to 37; these studies, with supporting evidence of tobacco-specific carcinogens in the body fluid of passive smokers confirm the carcinogenicity of SHS (Hackshaw et al., 1997). Despite press reports to the contrary, the recent WHO study by Boffetta et al.(1997) is completely consistent with these earlier studies.
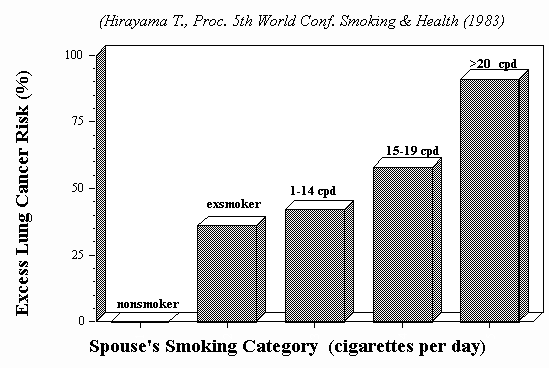
The body of evidence from spousal smoking studies suggests that the average excess risk of lung cancer from passive smoking is 24% (95% CI: 13% to 36%) [Hackshaw et al., 1997]. However, for nonsmokers exposed to the smoke of a pack of cigarettes per day or more, the risk increase can be considerably greater; the EPA summarized 12 studies that assessed this risk. For 9 studies in 5 countries, the risk in this category ranged from 57% to 220%; 3 other studies in 2 countries reported risks in the 10% to 20% range (U.S. EPA, 1992, Table 5-11). In the U.S. in 1980, the average smoker smoked 32 cigarettes per day (Repace and Lowrey, 1980). The large cohort study by Hirayama (1983) exemplifies the dose-response trend (Figure 1, below). The lack of completely unexposed controls depresses odds ratios (Repace and Lowrey, 1985). Hirayama’s controls may suffer less from this problem than studies in other cultures due to the traditional exclusion of Japanese women from non-domestic workplaces. A lung cancer observed in the 1980’s and 1990’s is generally the result of 20 to 40 years’ SHS exposure, dating back to 1940’s to the 1970’s when few restrictions on smoking existed in most workplaces, homes, or restaurants.
Strong evidence of the hazard of secondhand smoke also comes from studies of smokers. In the United States and other developed countries, cigarette smoking causes most cases of lung cancer and chronic obstructive pulmonary disease, and a substantial fraction of coronary heart disease deaths (Thun et al., 1997). Smokers suffer increased rates of cancers of the lung, larynx, oral cavity esophagus, bladder, kidney, urinary tract, and pancreas (NCI Monograph 8, Preface, 1997).In the largest and most recent study of active smokers, the American Cancer Society’s study of more than 1 million men and women, among active cigarette smokers, 52% of all male deaths and 43% of all female deaths are attributed to their smoking (Thun et al., 1997). Of those smokers who die from smoking, 55% die in middle age (i.e., from 35 yr. to 69 yr.). Of those who die in middle age, 22 years of life expectancy are lost, and of those who die in old age, 8 years of life are lost (Peto, Lopez et al., 1994) In other words, half of those who deliberately inhale cigarette smoke die from it. More than half of those die in the prime of life.
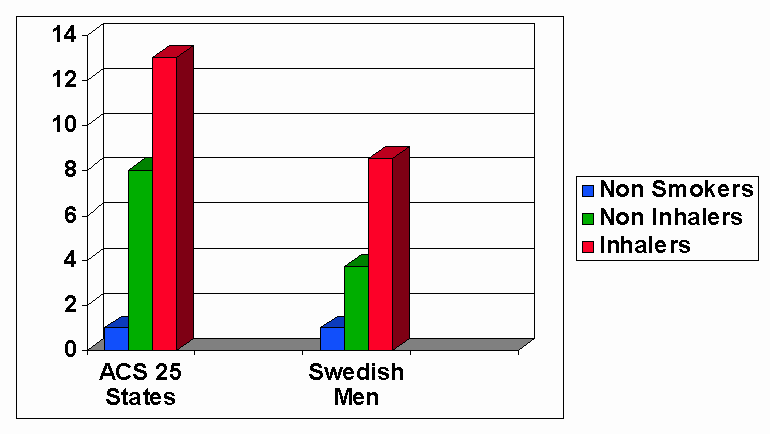
Given the enormous toxicity of tobacco smoke, is it reasonable to presume that breathing any amount of secondhand smoke can possibly do no harm? Can it be presumed that lower levels of exposure, such as encountered in passive smoking are safe? The most heavily exposed passive smokers are active smokers who do not inhale. Figure 2 below shows the relative lung cancer risks (from right to left, respectively) for nonsmokers, smokers who do not inhale, and smokers who inhale (SG, 1979). Similarly, cigar smokers who do not inhale suffer major, statistically significant increases in cancer of the larynx (relative risk, 10.6), cancer of the lung (1.97), cancer of the pancreas (1.55), sites which are distal to the oral cavity and pharynx (6.98). Moreover, many of the compounds in tobacco smoke are known occupational carcinogens, such as arsenic (lung), benzene (blood), vinyl chloride (liver, brain), 2-napthalymine and 4-aminobiphenyl (bladder). In fact, in the United States, arsenic, benzene, and vinyl chloride are regulated hazardous air pollutants, and the latter two bladder carcinogens are banned in dye manufacture. This evidence is sufficient by itself to indict secondhand smoke as a hazardous substance to be avoided.
[ Abstract ]
Introduction
[ Secondhand Smoke and Cardiovascular Disease ]
[ Secondhand Smoke Exposure ]
[ Smoke-Free Restaurant Laws ]
[ SHS Lessons from California ]
[ Conclusions ]
[ Technical Appendices ]